Next time you hear someone use the phrase “death panels,” ask them if they’re aware of a study of terminally ill lung cancer patients which appeared in the New England Journal of Medicine in 2010. It showed that those who chose palliative care and hospice lived three months longer and had a better quality of life, with fewer side effects, than those who opted for aggressive treatment.
If those same people talk about the need to control government spending on health care, you might point them to the 2007 study by the National Hospice and Palliative Care Organization, which claimed Medicare saved over $2,300 for every patient who opted for palliative and hospice care when diagnosed with a terminal illness.
RELATED: Life at All Costs: The Mid Death Crisis
Yet fewer than 40 percent of U.S. cancer patients who eventually died from the disease used hospice or palliative care services in 2007, which in two out of three cases were delivered in the person’s home or nursing home. A third of the patients didn’t get the referral for hospice services until a week before their deaths, and the median length of time in hospice was just three weeks.
“People should have a discussion about hospice three to six months before death, not three weeks (beforehand),” Thomas J. Smith, director of palliative care at Johns Hopkins University’s Sidney Kimmel Comprehensive Cancer Center, told this past weekend’s American Society of Clinical Oncologists (ASCO) annual meeting, held in Chicago. “This is fairly easy to predict.”
The 30,000-strong organization, which represents the physicians who will treat the more than 1.6 million people who will be diagnosed with cancer in 2012, is under increasing pressure to cut costs. ASCO was one of nine medical specialty groups that announced earlier this year that it would recommend five drugs, tests and procedures that are overused and waste scarce health care system resources.
At the top of ASCO’s list was cutting off expensive chemotherapy when patients with fast-spreading solid tumors continued to deteriorate after receiving their first or second drug regimens for their disease. Over 577,000 people will die this year from the more than 100 forms of cancer.
The latest FDA-approved drugs given to such patients – drugs that can cost $100,000 or more in that last year of treatment – often extend life by only a few weeks or months. Those results were often demonstrated in clinical trials with patients who were more likely to benefit because they had few or no other serious health conditions like heart disease or diabetes. “Effectiveness in a trial does not necessarily translate into effectiveness in the community,” Smith said.
There are numerous roadblocks to creating more realistic expectations about what modern medicine can do for terminally ill patients. Not all of them are foisted on the health care system by political scare tactics, such as the Republican Party-led assault on President Obama’s health care reform law during the 2010 election season, which slapped the “death panel” label on its provision that encouraged physicians to discuss end-of-life care with their patients.
For instance, numerous surveys have shown that physicians and patients shy away from having end-of-life care conversations. The National Cancer Institute website on pancreatic cancer never mentions that the disease is fatal for almost everyone within two years. Cancer centers in most large urban areas are increasingly turning to advertising to lure patients to their latest and usually most expensive services such as robotic surgery, which has never been demonstrated as superior to conventional surgery.
“This isn’t marketing, it’s propaganda,” said Richard Sullivan, a practicing oncologist at King’s Health Partners in Great Britain. “People are very sensitive to messages delivered in this manner. In Europe it is not allowed, and if I were running public policy in the U.S., I would simply ban it.”
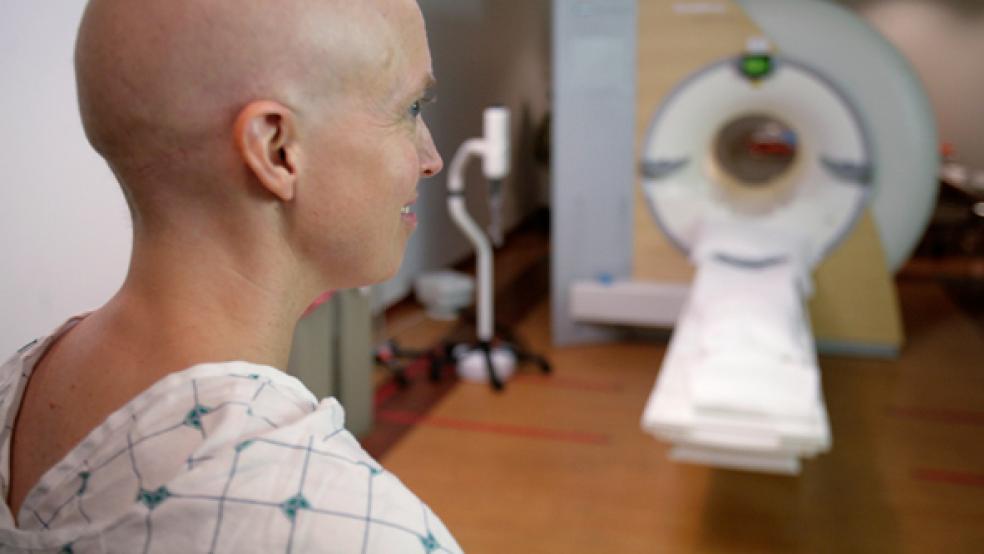
The rest of ASCO’s “top five” list for oncologists focused on imaging and the overuse of one drug. Oncologists were told not to order expensive CT or PET scans for early stage prostate and breast cancer patients whose small tumors haven’t spread to other organs or surrounding tissues. They also cautioned against using the imaging tests routinely in asymptomatic patients whose early stage breast cancer had been successfully treated. “Radiation poses its own cancer risk,” Smith noted.
The final recommendation called for cutting back on the use of Amgen’s Neupogen, a white blood-cell stimulating factor given to patients undergoing chemotherapy to reduce the risk of infection. “The U.S. uses 75 percent of the world supply (of this drug), which accounted for $3.6 billion in sales before mark-up,” Smith said. “Over half was given in an inappropriate way.”