With Alaska Gov. Bill Walker’s decision late last week to unilaterally accept federal funds available to cover low-income people under the Affordable Care Act, three-fifths of all the states have now accepted expanded Medicaid benefits for their residents.
Three years after the Supreme Court limited the expansion of Medicaid under President Obama’s health care reform law, the federal-state health program for the poor and disabled has evolved into a troubling dual system in which the availability of health care is being determined largely by the continued partisan divide over Obamacare and the geographic accident of where poor people happen to live.
Related: Soaring Medicaid Enrollment Could Hit State Budgets
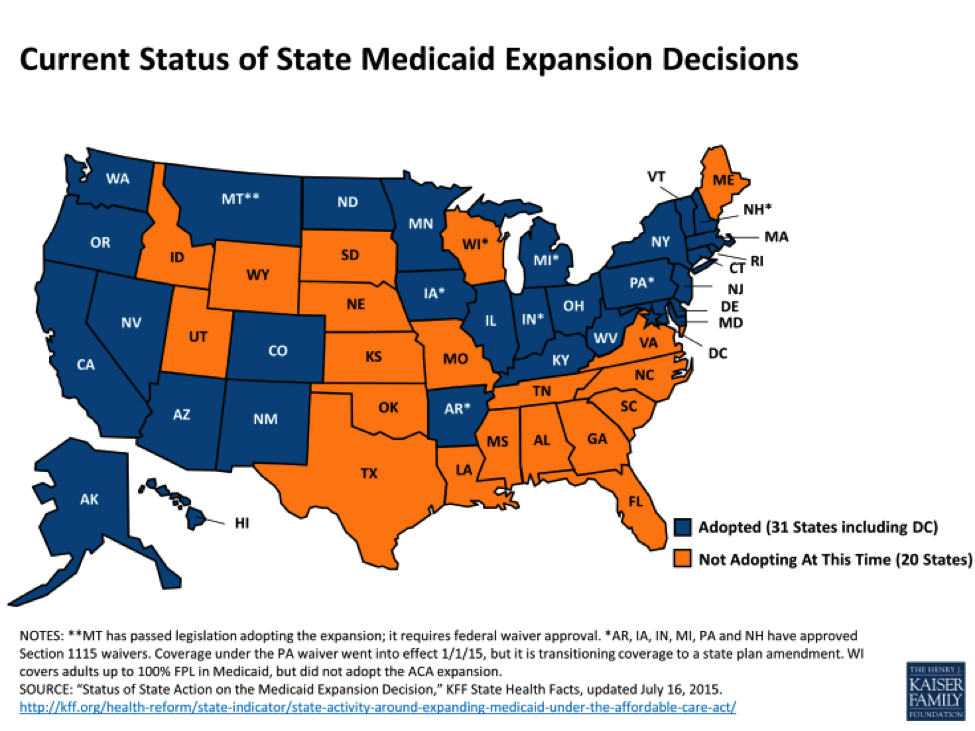
Once they were free to decide for themselves whether to go along with expanding Medicaid coverage, 30 states and the District of Columbia ultimately agreed to the coverage. But the 20 remaining states — many of them dominated by Republican state legislatures or statehouses — have either rejected the offer or are leaning against it. The result is that poor people living in Arkansas, for example, can qualify for expanded Medicaid coverage, while people in equally dire financial straits living in the adjoining states of Oklahoma, Missouri, Tennessee and Mississippi cannot.
The ACA expands Medicaid coverage for most adults with income up to 138 percent of the federal poverty level. More than 15 million men, women and children have become eligible for Medicaid in states that participate in the expansion, according to the White House. Roughly 5 million others are being denied coverage because of decisions by their states to reject the offer.
Alaska’s Walker, an independent who took office last December, told reporters in Anchorage on Thursday that he could not wait any longer to offer health coverage to approximately 42,000 people his administration projects will be eligible under the expansion. The governor acted on his own after failing to persuade his legislature to go along with the program, although he hopes the state’s Legislative Budget and Audit Committee concurs within 45 days.
For states that agree to extend health care coverage to low income people who for a variety of reasons haven’t qualified for Medicaid until now, the federal government will cover the full cost through 2016 and then gradually lower its share to 90 percent by 2020. State officials estimate Alaska would draw $1.1 billion in additional federal funds over the next six years.
While most governors or their legislatures concluded this was a good deal for their states — including Republican chief executives in Ohio and Kentucky — others rejected it either because they oppose Obamacare or because they fear the federal government will eventually leave them holding the bag for the entire cost of the expanded coverage.
Americans for Prosperity, a conservative advocacy group financed by the billionaire Koch brothers, waged an aggressive campaign in Alaska against the expansion, warning residents that it posed a long-term financial threat to the state.
“At a time when the state is facing a $4 billion deficit, we think it's a bad idea to add 40,000 people to the program,” AFP Alaska State Director Jeremy Price said, according to media reports.
However, Patrick Willard, Families USA’s Health Action Director, hailed Walker’s decision and said that the focus now shifts to Utah, where Republican Gov. Gary Herbert and legislative leaders just agreed on the framework for expanding Medicaid coverage in the state.
Related: States of Health: Winners & Losers in Medicaid
“We know that expanding health care access is bringing down the uninsured rates and helping states achieve budget savings,” Willard said in a statement. “The bad news is that too many states with lots of uninsured are holding out for political reasons.”
Here is a map showing the great divide between states with and without expanded Medicaid coverage: