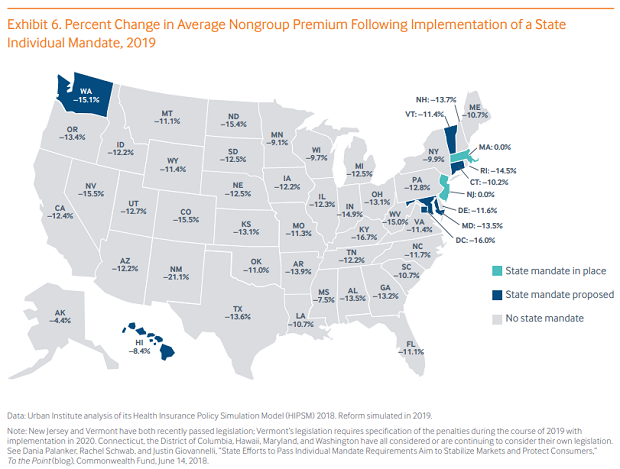
Health insurance premiums in the federal marketplace would cost 11.8 percent less in 2019 if all 50 states adopted coverage mandates, according to a new study from the Commonwealth Fund and the Urban Institute. Additionally, 3.9 million more Americans would be covered by insurance next year, and 7.5 million in 2022, compared to projections under current law.
The mandate requiring individuals to have health insurance was imposed at the federal level by the Affordable Care Act but effectively eliminated by the Republican tax law starting in 2019. The end of the mandate, which was controversial politically, comes with a significant cost in terms of lower coverage levels and higher premiums. According to the Congressional Budget Office, 3 million fewer people will have health insurance in 2019 as result of eliminating the individual mandate penalties, and premiums in the individual marketplaces will rise by roughly 15 percent.
The mandate was designed to bring more healthy people into the insurance pool, thereby lowering the overall cost of care. Some states are looking into imposing their own mandates in order to boost enrollment and reduce costs, and Massachusetts and New Jersey have already done so. The Commonwealth study projected changes in overall coverage and cost that would result if all of the states imposed individual mandate penalties, although there is no indication that a substantial number of states are planning to do so.