Obamacare’s Dirty Secret: 31 Million Still Can’t Afford Treatment
The president’s healthcare law sliced America’s uninsured rate down to historic lows by expanding coverage for tens of millions of Americans. At the same time, however, the number of insured people who still lack affordable, robust coverage is rising sharply as more people buy into high-deductible policies.
A new study from the Commonwealth Fund reveals that about 23 percent of Americans with coverage are considered underinsured—up from 12 percent in 2003. That means roughly 31 million Americans who bought health insurance still have trouble affording treatment under their policies.
The researchers at the Commonwealth Fund defined “underinsured” people as having out-of-pocket costs that total 10 percent or more of their annual income, or a deductible that is 5 percent or more of their income. The study concluded that high-deductible policies are likely the culprit behind this massive influx of underinsured people.
The findings are a huge problem for the Obama administration since the entire goal was to expand access to coverage to millions of Americans that they presumably would use instead of delaying treatment. But a handful of recent studies show that even people with health insurance are delaying treatment because they can’t afford it.
Related: High Deductible Plans Have More People Delaying Treatment
A December Gallup Poll showed at least 38 percent of insured, middle-income people, said they had delayed medical treatment because of the cost. “While many Americans have gained insurance, there has been no downturn in the percentage who say they have had to put off needed medical treatment because of cost,” Gallup’s Rebecca Riffkin wrote in a post on the pollster’s website.
The shift toward cost-sharing and high-deductible policies—defined by the Internal Revenue Service as those with annual deductibles of $1,300 or more for individuals and $2,600 for families--is widespread among exchange policies but also employer plans.
The Commonwealth Foundation’s study, unsurprisingly, reveals that low-income people with coverage are about twice as likely to be “underinsured” than people earning more than 200 percent of the poverty line.
Of course, it’s important to note that while affordability continues to be an issue, significantly more people do have health insurance because of the law.
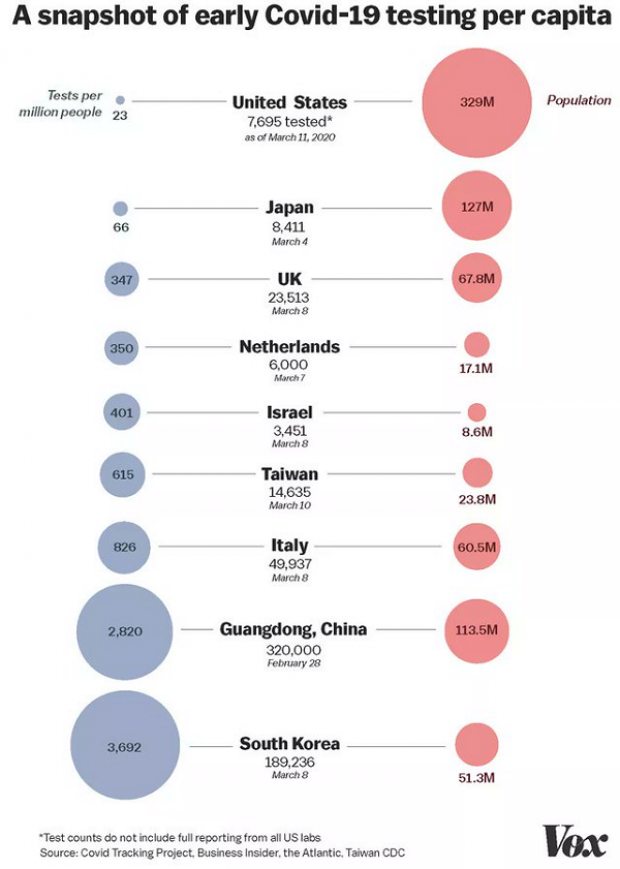
Chart of the Day: Long Way to Go on Coronavirus Testing

The White House on Friday unveiled plans for a new effort to ramp up testing for Covid-19, which experts say is an essential part of limiting the spread of the virus. This chart from Vox gives a sense of just how far the U.S. has to go to catch up to other countries that are dealing with the pandemic, including South Korea, the leading virus screener with 3,692 tests per million people. The U.S., by comparison, has done about 23 tests per million people as of March 12.
After Spending $2 Billion, Air Force Bails Out on Planned Upgrades of B-2 Bombers

The Air Force has scrapped a planned upgrade of its B-2 stealth bomber fleet — even after spending $2 billion on the effort — because defense contractor Northrup Grumman didn’t have the necessary software expertise to complete the project on time and on budget, Bloomberg’s Anthony Capaccio reports, citing the Pentagon’s chief weapons buyer.
Ellen Lord, the undersecretary of defense for acquisition and sustainment, told reporters that the nearly $2 billion that had already been spent on the program wasn’t wasted because “we are still going to get upgraded electronic displays.”
Big Hurdle for Sanders’ Plan to Cancel Student Debt

Bernie Sanders wants to eliminate $1.6 trillion in student debt, to be paid for by a tax on financial transactions, but doing so won’t be easy, says Josh Mitchell of The Wall Street Journal.
The main problem for Sanders is that most Americans don’t support the plan, with 57% of respondents in a poll last fall saying they oppose the idea of canceling all student debt. And the politics are particularly thorny for Sanders as he prepares for a likely general election run, Mitchell says: “Among the strongest opponents are groups Democrats hope to peel away from President Trump: Rust Belt voters, independents, whites, men and voters in rural areas.”
Number of the Day: $7 Million

That’s how much Michael Bloomberg is spending per day in his pursuit of the Democratic presidential nomination, according to new monthly filings with the Federal Election Commission. “In January alone, Bloomberg dropped more than $220 million on his free-spending presidential campaign,” The Hill says. “That breaks down to about $7.1 million a day, $300,000 an hour or $5,000 per minute.”