Obamacare’s Dirty Secret: 31 Million Still Can’t Afford Treatment
The president’s healthcare law sliced America’s uninsured rate down to historic lows by expanding coverage for tens of millions of Americans. At the same time, however, the number of insured people who still lack affordable, robust coverage is rising sharply as more people buy into high-deductible policies.
A new study from the Commonwealth Fund reveals that about 23 percent of Americans with coverage are considered underinsured—up from 12 percent in 2003. That means roughly 31 million Americans who bought health insurance still have trouble affording treatment under their policies.
The researchers at the Commonwealth Fund defined “underinsured” people as having out-of-pocket costs that total 10 percent or more of their annual income, or a deductible that is 5 percent or more of their income. The study concluded that high-deductible policies are likely the culprit behind this massive influx of underinsured people.
The findings are a huge problem for the Obama administration since the entire goal was to expand access to coverage to millions of Americans that they presumably would use instead of delaying treatment. But a handful of recent studies show that even people with health insurance are delaying treatment because they can’t afford it.
Related: High Deductible Plans Have More People Delaying Treatment
A December Gallup Poll showed at least 38 percent of insured, middle-income people, said they had delayed medical treatment because of the cost. “While many Americans have gained insurance, there has been no downturn in the percentage who say they have had to put off needed medical treatment because of cost,” Gallup’s Rebecca Riffkin wrote in a post on the pollster’s website.
The shift toward cost-sharing and high-deductible policies—defined by the Internal Revenue Service as those with annual deductibles of $1,300 or more for individuals and $2,600 for families--is widespread among exchange policies but also employer plans.
The Commonwealth Foundation’s study, unsurprisingly, reveals that low-income people with coverage are about twice as likely to be “underinsured” than people earning more than 200 percent of the poverty line.
Of course, it’s important to note that while affordability continues to be an issue, significantly more people do have health insurance because of the law.
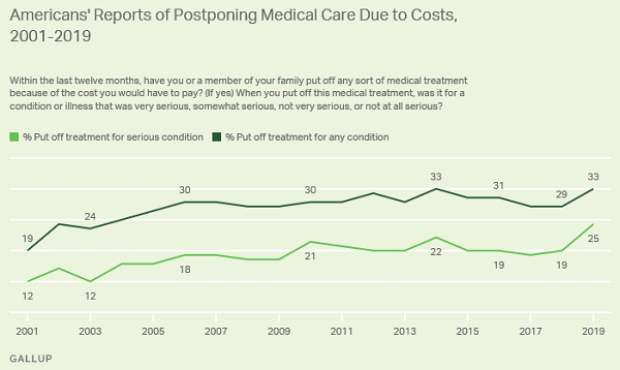
Increasing Number of Americans Delay Medical Care Due to Cost: Gallup

From Gallup: “A record 25% of Americans say they or a family member put off treatment for a serious medical condition in the past year because of the cost, up from 19% a year ago and the highest in Gallup's trend. Another 8% said they or a family member put off treatment for a less serious condition, bringing the total percentage of households delaying care due to costs to 33%, tying the high from 2014.”
Number of the Day: $213 Million

That’s how much the private debt collection program at the IRS collected in the 2019 fiscal year. In the black for the second year in a row, the program cleared nearly $148 million after commissions and administrative costs.
The controversial program, which empowers private firms to go after delinquent taxpayers, began in 2004 and ran for five years before the IRS ended it following a review. It was restarted in 2015 and ran at a loss for the next two years.
Senate Finance Chairman Chuck Grassley (R-IA), who played a central role in establishing the program, said Monday that the net proceeds are currently being used to hire 200 special compliance personnel at the IRS.
US Deficit Up 12% to $342 Billion for First Two Months of Fiscal 2020: CBO

The federal budget deficit for October and November was $342 billion, up $36 billion or 12% from the same period last year, the Congressional Budget Office estimated on Monday. Revenues were up 3% while outlays rose by 6%, CBO said.
Hospitals Sue to Protect Secret Prices

As expected, groups representing hospitals sued the Trump administration Wednesday to stop a new regulation would require them to make public the prices for services they negotiate with insurers. Claiming the rule “is unlawful, several times over,” the industry groups, which include the American Hospital Association, say the rule violates their First Amendment rights, among other issues.
"The burden of compliance with the rule is enormous, and way out of line with any projected benefits associated with the rule," the suit says. In response, a spokesperson for the Department of Health and Human Services said that hospitals “should be ashamed that they aren’t willing to provide American patients the cost of a service before they purchase it.”
See the lawsuit here, or read more at The New York Times.
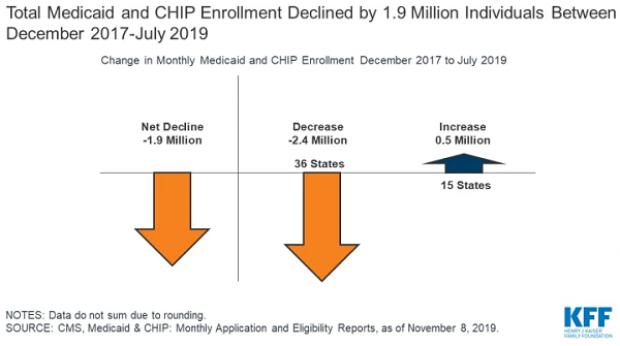
A Decline in Medicaid and CHIP Enrollment
Between December 2017 and July 2019, enrollment in Medicaid and the Children's Health Insurance Program (CHIP) fell by 1.9 million, or 2.6%. The Kaiser Family Foundation provided an analysis of that drop Monday, saying that while some of it was likely caused by enrollees finding jobs that offer private insurance, a significant portion is related to enrollees losing health insurance of any kind. “Experiences in some states suggest that some eligible people may be losing coverage due to barriers maintaining coverage associated with renewal processes and periodic eligibility checks,” Kaiser said.