Medical ID Theft is a Way Bigger Problem Than You Think

Forget Target and Home Depot. You may be risking identity theft every time you visit the doctor’s office.
Medical ID theft, in which thieves steal your Social Security number and health insurance info in order to fraudulently obtain medical services or treatment, is skyrocketing.
More than 90 percent of healthcare organizations have had a data breach, and 40 percent had more than five data breaches in the past two years, according to a report released last month by ID Experts. Attacks by criminal organizations are up 125 percent over the past five years. Medical identities are worth far more on the black market than financial identities.
The study estimates that data breaches may have cost the industry $6 billion in the last two years. The scariest stat for consumers: Half of organizations surveyed have little or no confidence in their ability to detect all patient data loss or theft.
Related: Now You Could Lost Your Medical Identity, Too
Victims of medical ID theft spend thousands to restore their credit and correct inaccuracies in their medical records, and unlike banks and credit card issuers, most healthcare organizations offer no protection services for victims.
In addition to the financial toll, there are health risks to victims of medical ID theft. If someone steals your identity and receives treatment that gets added to your medical records, doctors may have incorrect information regarding your health history and allergies.
It’s difficult to prevent medical ID theft, but monitoring your credit and closely reading your healthcare bill and explanation of benefits notices can help you catch it early.
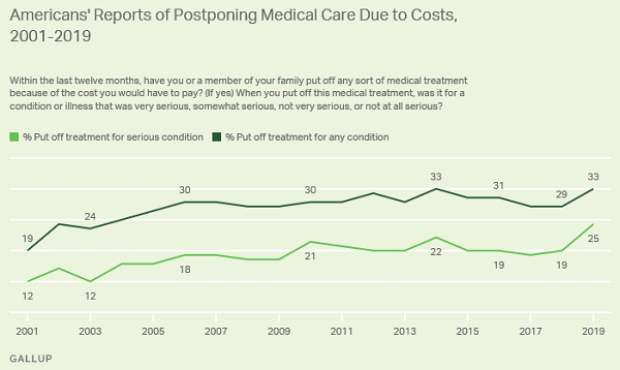
Increasing Number of Americans Delay Medical Care Due to Cost: Gallup

From Gallup: “A record 25% of Americans say they or a family member put off treatment for a serious medical condition in the past year because of the cost, up from 19% a year ago and the highest in Gallup's trend. Another 8% said they or a family member put off treatment for a less serious condition, bringing the total percentage of households delaying care due to costs to 33%, tying the high from 2014.”
Number of the Day: $213 Million

That’s how much the private debt collection program at the IRS collected in the 2019 fiscal year. In the black for the second year in a row, the program cleared nearly $148 million after commissions and administrative costs.
The controversial program, which empowers private firms to go after delinquent taxpayers, began in 2004 and ran for five years before the IRS ended it following a review. It was restarted in 2015 and ran at a loss for the next two years.
Senate Finance Chairman Chuck Grassley (R-IA), who played a central role in establishing the program, said Monday that the net proceeds are currently being used to hire 200 special compliance personnel at the IRS.
US Deficit Up 12% to $342 Billion for First Two Months of Fiscal 2020: CBO

The federal budget deficit for October and November was $342 billion, up $36 billion or 12% from the same period last year, the Congressional Budget Office estimated on Monday. Revenues were up 3% while outlays rose by 6%, CBO said.
Hospitals Sue to Protect Secret Prices

As expected, groups representing hospitals sued the Trump administration Wednesday to stop a new regulation would require them to make public the prices for services they negotiate with insurers. Claiming the rule “is unlawful, several times over,” the industry groups, which include the American Hospital Association, say the rule violates their First Amendment rights, among other issues.
"The burden of compliance with the rule is enormous, and way out of line with any projected benefits associated with the rule," the suit says. In response, a spokesperson for the Department of Health and Human Services said that hospitals “should be ashamed that they aren’t willing to provide American patients the cost of a service before they purchase it.”
See the lawsuit here, or read more at The New York Times.
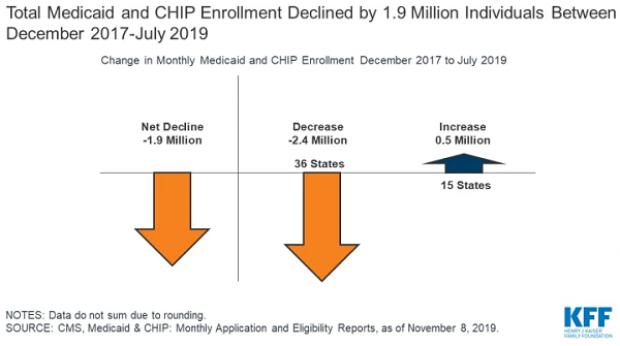
A Decline in Medicaid and CHIP Enrollment
Between December 2017 and July 2019, enrollment in Medicaid and the Children's Health Insurance Program (CHIP) fell by 1.9 million, or 2.6%. The Kaiser Family Foundation provided an analysis of that drop Monday, saying that while some of it was likely caused by enrollees finding jobs that offer private insurance, a significant portion is related to enrollees losing health insurance of any kind. “Experiences in some states suggest that some eligible people may be losing coverage due to barriers maintaining coverage associated with renewal processes and periodic eligibility checks,” Kaiser said.