In the ongoing struggle of policy makers to contain government health care costs, one of the most perplexing challenges has been coping with often huge variations in Medicare spending throughout the country.
The government’s cost for providing the same Medicare services to seniors can vary by thousands of dollars, depending on where they live.
Related: 4 Ways to Get Cheaper Medications as Drug Prices Soar
The controversy dates back to 2009, during the congressional debate on Obamacare when a New Yorker article by Atul Gawande explored why some communities in the U.S. –including McAllen, Texas – have much higher health care costs that other regions. Gawande concluded that these increased costs were likely due to the culture of medical practice in the region, which resulted in more unnecessary and costly care and procedures.
A study released late last week by the Kaiser Family Foundation tells the story:
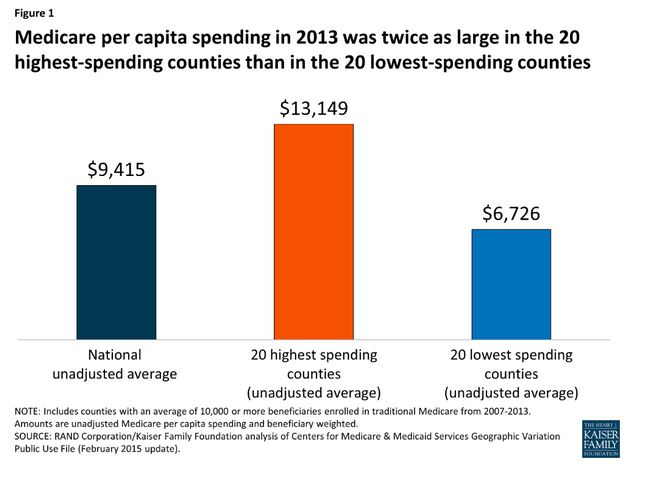
Although Medicare per capita spending nationwide averaged $9,415 in 2013, per capita spending on average totaled $13,140 in 20 counties with the highest levels, but only $6,726 in the 20 counties with the lowest levels.
As the chart below illustrates, Medicare per capita spending in 2013 was twice as large in the 20 highest-spending counties than in the 20 lowest-spending counties.
Related: Millions Face a 50 % Medicare Premium Hike If Obama and Congress Don’t Act
The 20 counties with the highest unadjusted Medicare per capita spending in 2013 were primarily located in the Northeast, Mid-Atlantic and the South. In contrast, most of the counties with the lowest per capita spending were in the West.
For years, researchers have argued that the differences in Medicare spending across the country were prompted by variances in the way doctors and hospitals treated and billed their patients – with some ordering inordinate numbers of medical tests or failing to coordinate the medical services. Experts believed that many of those problems and excesses could be overcome by “policy interventions,” such as change in the financial incentives for health care providers.
But other researchers have argued, in effect, that “geography is destiny” and that much of the variation in cost has to do with the beneficiaries’ general health and socio-economic status, as well as how frequently areas residents require costly hospitalization and post-operative services.
While the report doesn’t take a stand on the predominant factor, these vastly different regional costs may well become an issue when and lawmakers finally tackle additional health care reform.
Related: Millions Facing a Hefty Increase in Medicare Premiums in 2016
The 2010 Affordable Care Act included a number of provisions designed to encourage greater efficiency in the delivery of care for Medicare beneficiaries by modifying incentives for providers to reduce excess costs and improve quality of care – and they may have contributed to bringing down costs in some areas.
Yet even with such efforts, deep differences in per capita Medicare costs persist throughout the country.
“We did do an analysis that suggests the gap between the highs and the lows has narrowed,” said Tricia Neuman, a senior vice president at the Kaiser Family Foundation and the director of its Program on Medicare Policy. “The fact that it’s narrowed raises interesting questions as to why that has occurred” but the study stopped short of advancing a theory.
“The Affordable Care Act may well have been a factor and some of the other initiatives that have been put out,” she added. “For example, we saw a narrowing with respect to durable medical equipment spending, and there was a competitive bidding effort that the administration did. And there was some narrowing with respect to home health services.”
“But we really didn’t set out to do any causal analysis,” she said.
While the study’s authors avoided clear conclusions about the factors at play in creating the geographic cost disparities, it does provide a detailed look at the typical high-cost county
Here are four brief factors that help to explain the counties with the costliest Medicare costs:
- The 20 counties had sicker and poorer beneficiary populations, on average, and a substantially greater share of black and Hispanic beneficiaries.
- Hospital inpatient care is more than twice as higher than in the lowest-spending counties.
- The counties also stand out for having more post-acute care providers per capita and fewer physicians than the 20 lowest-spending counties.