When the Occupy Wall Street movement emerged as the voice of the “99 percent” of Americans who were hit hardest by the Great Recession, the protest put a spotlight on big banks and financial service companies. They were ultimately responsible for the housing crisis that cost millions their homes, their jobs and their savings.
Some of the banks were dicing and splicing subprime mortgages into what were ersatz mortgages and selling them to other banks in the U.S. and globally. In short, they were pushing snake oil, which ultimately led to a massive number of new federal banking regulations — good and bad — and put a laser focus on income disparity and greed.
Related: How Big Pharma Lobbyists Make the Opioid Crisis Worse
Today, except for the recent Wells Fargo mess, the banks have been swept off the front pages by another business sector — the pharmaceutical industry.
It’s not just that drug companies have lobbied state lawmakers to resist legal restrictions on OxyContin, Vicodin and Fentanyl — three addictive opioids connected to the heroin epidemic.
It’s not just that some “specialty drugs,” code for injectable biologics, have annual price tags for chronic conditions like arthritis and psoriasis that may exceed the average household income.
It’s that some drugs that have been on the market for years have seen price increases of 1,000 percent to 5,000 percent -- like Turing’s lifesaving Daraprim, now $750 a pill, or Mylan’s EpiPen, which went from $100 a few years ago to $608 for a two-pen set.
An estimated 15 million Americans have eczema, a common chronic skin condition made worse in dry weather. The skin itches, you scratch — and infections are common. Another common skin disorder, acne, affects about 80 percent of all people between the ages of 11 and 30 at some point, according to the National Institutes of Health.
Related: Epi-Pen Maker Enters the Pharmaceutical Industry’s Hall of Shame
Imagine you have one of these conditions, have been using medical creams for years, and then bingo: Your insurance company denies your claim because of a huge price increase, and your doctor has to scramble to find an equitable replacement.
Since 2009, the prices of prescription skin creams have quintupled or more. A report in The Washington Post last November said, “Of the 19 brand-name drugs included in the study, certain outliers showed massive price surges -- a 60-gram tube of a gel for a type of skin cancer increased from $1,686.78 for a tube to over $30,000. The gel is made by Valeant Pharmaceuticals, a company that has come under Senate investigation for its drug hiking practices.”
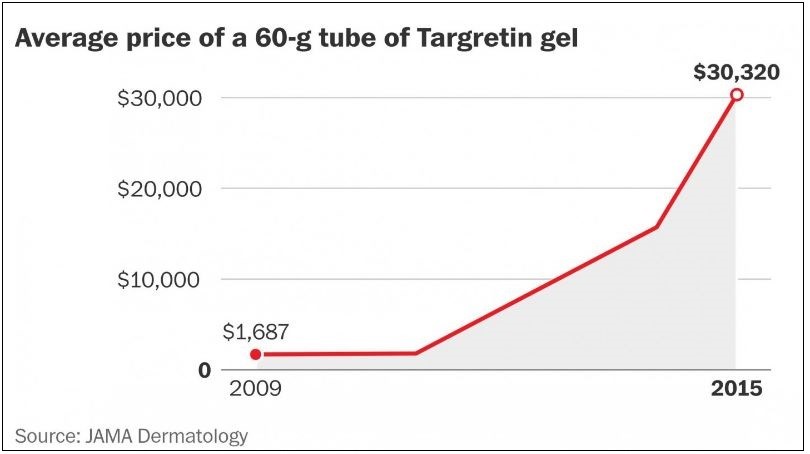
The Postpoints out that shortages of antibiotics had some effect on price increases, but after those shortages had been resolved, the prices did not come down. In fact, one private drugmaker based in Chicago, Novum Pharma, is now charging nearly $10,000 for a 60-gram tube of Aloquin Gel for the treatment of eczema and acne, an 1,100 percent increase from its already high price of $241.50.
Here’s the kicker: The gel is only “possibly effective,” which indicates the FDA is not exactly convinced that it works as intended.
Gouging? You bet. The good news in the case of Aloquin, at least, is that there are cheaper alternatives.
Related: Teva, World's Largest Generic Drugmaker, Looks to Get Even Bigger
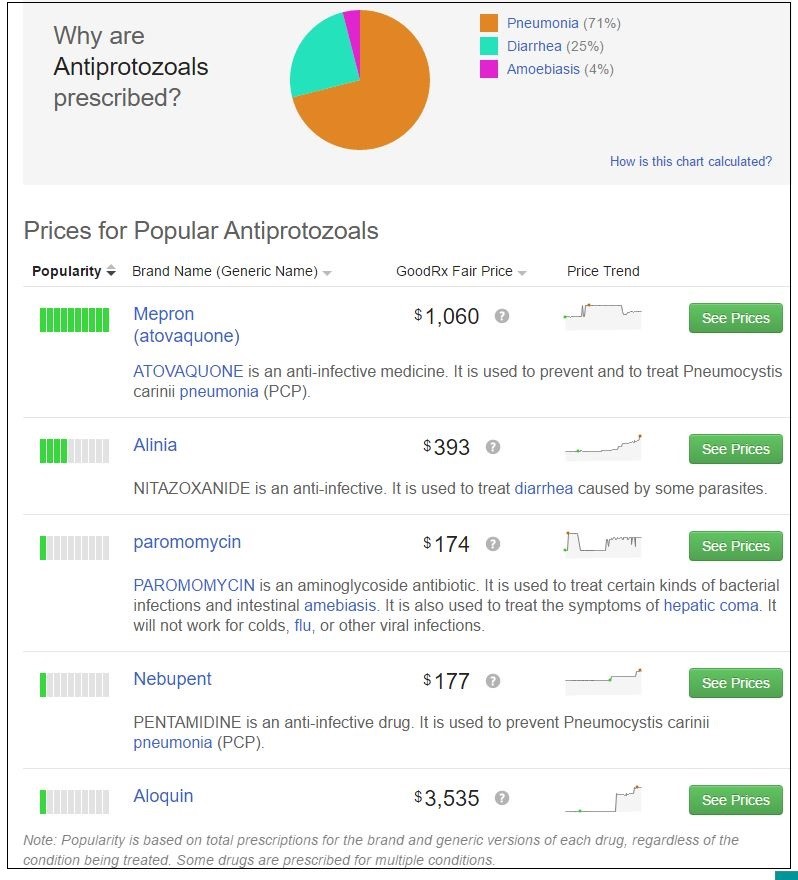
How do consumers, medical professionals, and the federal government fight this war on drug gouging? As in any battle, you have to know your strengths and how best to use them. However, you also need a full picture of the enemies’ position. An AP story last September 15th identified six reasons drug prices are going through the roof:
- Unlike other countries, Medicare/Medicaid does not set price controls.
- Patents are filed during testing, giving drugmakers a monopoly for roughly 12 years.
- Limited competition due to low profitability of generic drugs.
- Limited markets for expensive-to-produce drugs.
- Development and production costs; industry groups say it can take about a decade and well over $1 billion to get a new drug approved.
- Fewer generics due to fewer patent expirations.
Related: Want Lower Drug Prices? Start by Fixing the FDA
So what should we do?
The Federal Government: In the simplest terms, the open-ended payment structure of Medicare Part D has to go. In its place — negotiated prices, with some consideration for costly innovations. Also, the FDA needs to make innovative drug development less burdensome by eliminating some old, 20th-century regulations that no longer apply in a computer age.
Medical Professionals: First, hospitals have to stop wasting $3 billion worth of high-tech drugs each year. Doctors should stop taking money or trips from pharma companies since there is voluminous evidence that drug prescriptions increase as a result.
Insurance Companies: Insurance companies should negotiate reasonable prices for essential medications for their clients.
Consumers: The internet makes it easy to shop for the best prices on drugs. GoodRx is one site that does just that.





