A new Centers for Disease Control (CDC) report that deaths from Hepatitis-C reached a record level in 2014 is a wakeup call to policy makers and health care experts who are facing challenges in identifying and treating Americans suffering from the deadly liver disease – and finding the money to pay for it.
The CDC reported on Wednesday that there were 19,659 deaths in 2014 related to Hep-C, up slightly from 19,368 the previous year but still an all-time record. A second CDC study that was published online in Clinical Infectious Diseases revealed that the annual mortality rate from Hep-C in 2013 surpassed the total aggregate number of deaths from 60 other infectious diseases – including HIV and tuberculosis.
Related: As Valeant’s CEO Apologizes, the Rest of the Industry Keeps Hiking Drug Prices
CDC officials and other public health care and medical experts voiced optimism that the Hep-C mortality trend will begin to plateau and then decline with the introduction in recent years of new wonder drugs like Gilead Science’s Sovaldi and Harvoni. Dr. Ira Jacobson, a hepatitis specialist and chair of the Department of Medicine at Mount Sinai Beth Israel hospital in New York, told The New York Times yesterday that he was optimistic “that we’re going to make a major dent in the mortality much sooner than we have without these medications.”
But the onerous cost of those and other new drugs – which can cost as much as $1,000 per pill or more -- have begun to overwhelm the budgets of Medicare, Medicaid, the Department of Veterans Affairs, federal and state prison systems and other government agencies that provide medical care. In some cases, these agencies have begun to prioritize the patients most in need of the drugs and those who are consigned to long waiting lists.
“We continue to struggle with the high costs of the drugs and trying to figure out ways to bring the costs down so that we can cover more people,” said Matt Salo, executive director of the National Association of Medicaid Directors.
About 3.5 million Americans currently suffer from Hepatitis-C and roughly half are unaware of their infection, according to the CDC. And while the greatest problem until recently has been treating veterans and baby boomers who were born between 1945 and 1965, the heroin epidemic sweeping the country has produced a whole new generation of Hep-C victims who inject drugs and share needles.
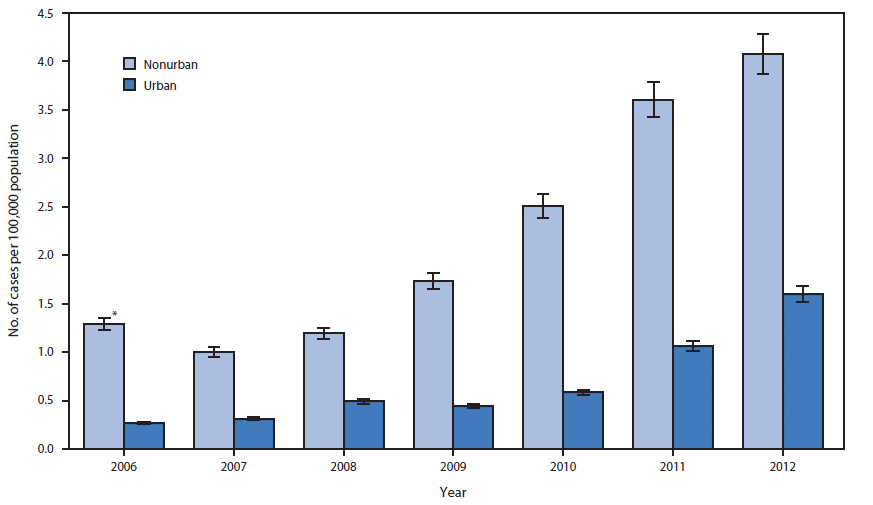
Source—Centers for Disease Control
Related: Ignoring Warnings, Drug Companies Hike Prices By 10 Percent
“Because hepatitis C often has few noticeable symptoms, the number of new cases is likely much higher than what is reported,” John W. Ward, director of CDC’s Division of Viral Hepatitis, said in a statement yesterday. “Due to limited screening and underreporting, we estimate the number of new infections is closer to 30,000 per year.”
“We must act now to diagnose and treat hidden infections before they become deadly and to prevent new infections,” he added.
Hepatitis-C is a serious liver infection caused by an often lethal virus, and it spreads from one person to another through contact with blood, including blood transfusions and shared needles. Gilead Sciences boasts that its two leading biologic medications have a cure rate of as high as 95 percent, in comparison with 40 percent for older, less advanced treatments. But Sovaldi and Harvoni can cost between $83,000 and $95,000 retail for a full course of treatment.
Under these massive costs, as many as three-fifths of state Medicaid programs have imposed tough restrictions on millions of low income patients and veterans seeking reimbursement for the treatment, as The Fiscal Times previously reported. Some 33 states spent more than $1 billion a year to treat the disease with Sovaldi, according to data released last December by members of the Senate. But even at that high level of spending, the funds were only sufficient to treat 2.4 percent of Medicaid patients who were infected with the virus, which often takes years before the liver is affected.
John Rother, CEO and President of the National Coalition on Health Care, an advocacy group that has been critical of the drug industry, warned in an interview today that the disease was clearly on the rise and that the government and the drug industry must reach an accommodation on how to address the health care and fiscal issues.
Related: Extreme Rise in Some Drug Prices Reaches a Tipping Point
Rother and other industry critics are pressing for reforms of the pharmaceutical industry, including ways to discourage drug companies like Gilead from acquiring the rights to drugs from other companies and then immediately doubling or even tripling the cost. The outgoing CEO of Valeant Pharmaceutical company recently apologized before a Senate committee on aging for engaging in such tactics.
“The medications are priced in a way that make it really difficult for people to afford the help they need and make it difficult for taxpayers to afford it, and raise costs for everyone,” Rother said. “We need to get to another place that would allow a more sustainable situation that still rewards the drug maker for innovation. But in this case, the drug maker didn’t innovate; it just bought the drug from another company and doubled the price.”
One good sign, according to Rother and Salo, is that more new Hepatitis-C drugs will be soon brought onto the market to create more competition for Gilead and, presumably, lower prices. Both Merck and Abbvie Pharmaceuticals reportedly have new drugs in the pipeline.
“Some folks are starting to say, you know what, once we get to three manufacturers in a space, that really gives us a lot more leverage to be able to bring prices down,” Salo said.